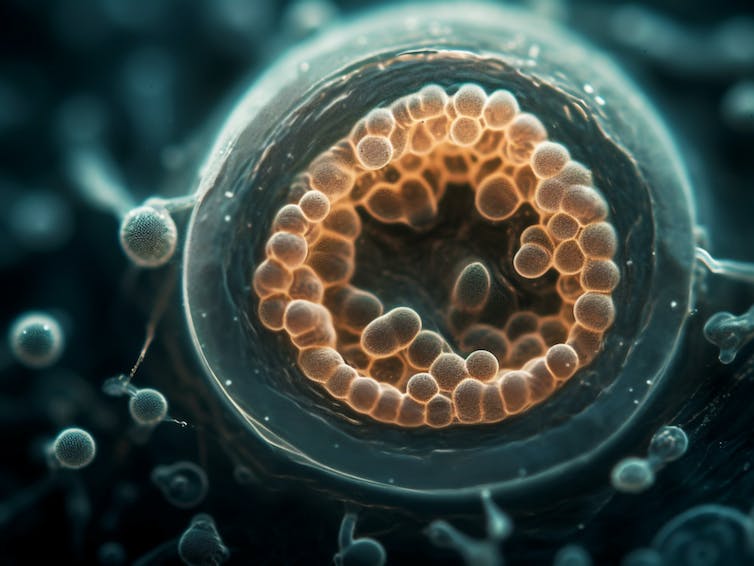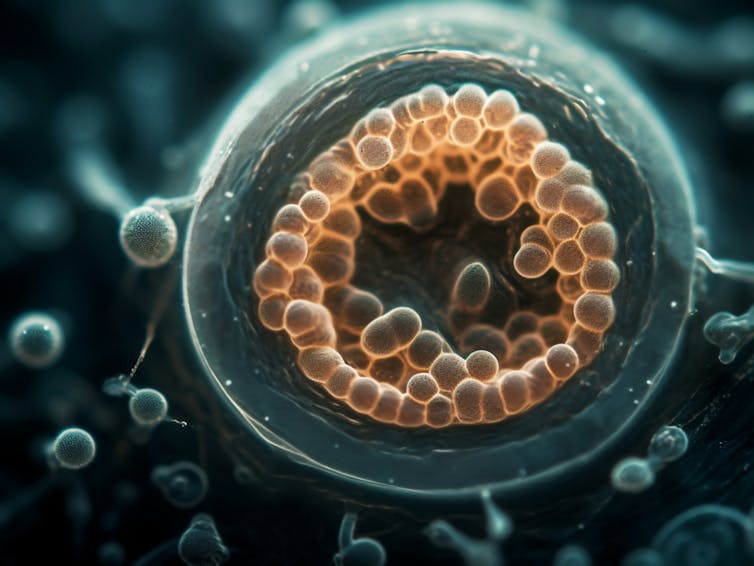
Juan Gaertner/Science Photo Library via Getty Images
Keith Latham, Michigan State University and Mary Faith Marshall, University of Virginia
Assisted reproductive technologies are medical procedures that help people experiencing difficulty having or an inability to have biological children of their own. From in vitro fertilization to genetic screening to creation of viable eggs from the skin cells of two male mice, each new development speaks to the potential of reproductive technologies to expand access to the experience of pregnancy.
Translating advances from the lab to the clinic, however, comes with challenges that go far beyond the purely technical.
Conversations around the ethics and implications of cutting-edge research often happen after the fact, when the science and technology have advanced beyond the point at which open dialogue could best protect affected groups. In the spirit of starting such cross-discipline conversations earlier, we invited developmental biologist Keith Latham of Michigan State University and bioethicist Mary Faith Marshall of the University of Virginia to discuss the ethical and technological potential of in vitro gametogenesis and assisted reproductive technology post-Roe.
How new are the ethical considerations raised by assisted reproductive technologies?
Keith
Every new technology raises many of the same questions, and likely new ones. On the safety and risk-benefit side of the ethical conversation, there’s nothing here that we haven’t dealt with since the 1970s with other reproductive technologies. But it’s important to keep asking questions, because the benefits are hugely dependent on the success rate. There are potential biological costs, but also possible social costs, financial costs, societal costs and many others.
Mary Faith
It’s probably been that way even longer. One of my mentors, Joseph Francis Fletcher, a pioneering bioethicist and Episcopal priest, wrote a book called “Morals and Medicine” in 1954. It was the first non-Roman Catholic treatment of bioethics. And he raised a lot of these issues there, including the technological imperative – the idea that because we can develop the technology to do something, we therefore should develop it.
Fletcher also said that the use of artifice, or human-made creations, is supremely human. That’s what we do: We figure out how things work and we develop new technologies like vaccines and heart-lung machines based on evolving scientific knowledge.
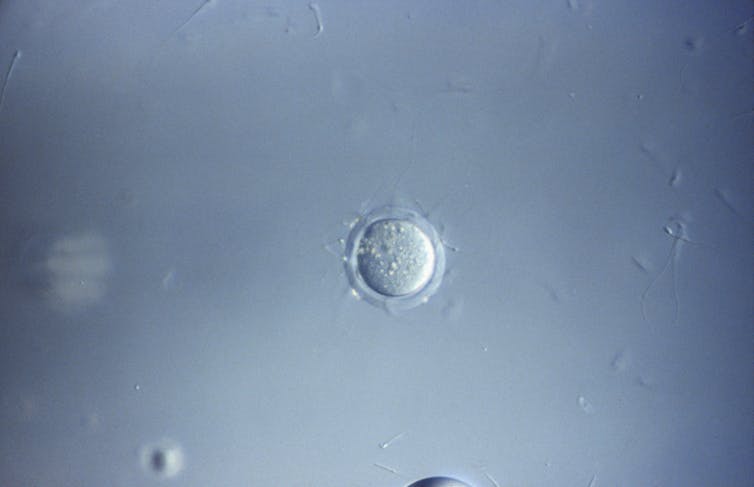
Clouds Hill Imaging Ltd./Corbis Documentary via Getty Images
I think that in most cases, scientists should be involved in thinking about the implications of their work. But often, researchers focus more on the direct applications of their work than the potential indirect consequences.
Given the evolution of assisted reproductive technology, and the fact that its evolution is going to continue, I think one of the central questions to consider is, what are the goals of developing it? For assisted reproduction, it’s to help infertile people and people in nontraditional relationships have children.
What are some recent developments in the field of assisted reproductive technology?
Keith
One recent advance in assisted reproductive technology is the expansion of pre-implantation genetic testing methods, particularly DNA sequencing. Many genes come in different variants, or alleles, that can be inherited from each parent. Providers can determine whether an embryo bears a “bad” allele that may increase the risk of certain diseases and select embryos with “healthy” alleles.
Genetic screening raises several ethical concerns. For example, the parents’ genetic profiles could be unwillingly inferred from that of the embryo. This possibility may deter prospective parents from having children, and such knowledge may also have potential effects on any future child. The cost of screening and potential need for additional cycles of IVF may also increase disparities.
There are also considerations about the accuracy of screening predictions without accounting for environmental effects, and what level of genetic risk is “serious” enough for an embryo to be excluded. More extensive screening also raises concerns about possible misuse for purposes other than disease prevention, such as production of “designer babies.”
At a genome-editing conference in March 2023, researchers announced that they were able to delete and duplicate whole chromosomes from the skin cells of male mice to make eggs. This method is one potential way to make eggs that do not carry genetic abnormalities.
They were very upfront that this was done at 1% efficiency in mice, which could be lower in humans. That means something bad happened to 99% of the embryos. The biological world is not typically binary, so a portion of that surviving 1% could still be abnormal. Just because the mice survived doesn’t mean they’re OK. I would say at this point, it would be unethical to try this on people.
As with some forms of genetic screening, using this technique to reduce the risk of one disease could inadvertently increase the risk of another. Determining that it is absolutely safe to duplicate a chromosome would require knowing every allele of every gene on that chromosome, and what each allele could do to the health of a person. That’s a pretty tall order, as that could involve identifying hundreds to thousands of genes, and the effects of all their variants may not be known.
Mary Faith
That raises the issue of efficacy and costs to yet another order of magnitude.
Keith
Genome editing with CRISPR technology in people carries similar concerns. Because of potential limitations in how precise the technology can be, it may be difficult for researchers to say they are absolutely 100% certain there won’t be off-target changes in the genome. Proceeding without that full knowledge could be risky.
But that’s where bioethicists need to come into play. Researchers don’t know what the full risk is, so how do you make that risk-benefit calculation?
Mary Faith
There’s the option of a voluntary global moratorium on using these technologies on human embryos. But somebody somewhere is still going to do it, because the technology is just sitting there, waiting to be moved forward.
How will the legal landscape affect the development and implementation of assisted reproductive technologies?
Mary Faith
Any research that involves human embryos is in some ways politicized. Not only because the government provides funding to the basic science labs that conduct this research, but because of the wide array of beliefs that members of the public at large have about when life begins or what personhood means.
The Dobbs decision, which overturned the constitutional right to an abortion, has implications for assisted reproduction and beyond. Most people who are pregnant don’t even know they’re pregnant at the earliest stages, and somewhere around 60% of those pregnancies end naturally because of genetic aberrations. Between 1973 and 2005, over 400 women were arrested for miscarriage in the U.S., and I think that number is going to grow. The implications for reproductive health care, and for assisted reproduction in the future, are challenging and frightening.
What will abortion restrictions mean for people who have multiple-gestation pregnancies, in which they carry more than one embryo at the same time? In order to have one healthy child born from that process, the other embryos often need to be removed so they don’t all die. In the past 40 years, the number of twin births doubled and triplet and higher-order births quadrupled, primarily because of fertility treatments.

Antonio Marquez lanza/Moment via Getty Images
Keith
IVF may transfer one, two, or sometimes three embryos at a time. The cost of care for preterm birth, which is one possible outcome of multiple-gestation pregnancies, can be high. That’s in addition to the cost of delivery. IVF clinics are increasingly transferring just one embryo to mitigate such concerns.
The life-at-conception bills that have been put forth in some U.S. state legislatures and Congress may contain language claiming they are not meant to prevent IVF. But the language of the bills could be extended to affect procedures such as IVF with pre-implantation genetic testing to detect chromosomal abnormalities, particularly when single-embryo transfer is the goal. Pre-implantation genetic testing has been increasing, with one study estimating that over 40% of all IVF cycles in the U.S. in 2018 involved genetic screening.
Could life-at-conception bills criminalize clinics that don’t transfer embryos known to be genetically abnormal? Freezing genetically abnormal embryos could avoid destroying them, but that raises questions of, to what end? Who would pay for the storage, and who would be responsible for those embryos?
How can we determine whether the risks outweigh the benefits when so much is unknown?
Keith
Conducting studies in animal models is an important first step. In some cases, it either hasn’t been done or hasn’t been done extensively. Even with animal studies, you have to recognize that mice, rabbits and monkeys are not human. Animal models may reduce some risks before a technology is used in people, but they won’t eliminate all risks, because of biological differences between species.
Mary Faith
We could look to the example of early recombinant DNA research in the U.S. The federal government created the Recombinant DNA Advisory Committee at the National Institutes of Health to oversee animal and early-phase human research involving synthetic or hybrid genetic material.
The death of Jesse Gelsinger, who was a participant in a gene therapy clinical trial in 1999, led to a halt in all gene therapy clinical trials in the U.S. for a time. When the Food and Drug Administration investigated what went wrong, they found huge numbers of adverse events in both humans and animals that should have been reported to the advisory committee but weren’t. Notably, the principal investigator of the trial was also the primary shareholder of the biotech company that made the drug being tested. That raises questions about the reality of oversight.
I think something like that earlier NIH advisory committee but for reproductive technologies would still be advisable. But researchers, policymakers and regulators need to learn from the lessons of the past to try to ensure that – especially in early-phase research – we’re very thoughtful about the potential risks and that research participants really understand what the implications are for participation in research. That would be one model for translating research from the animal into the human.
Bill West/AP Photo
Keith
A process to make sure that the people conducting studies don’t have a conflict of interest, like having the potential to commercially profit from the technology, would be useful.
Caution, consensus and cooperation should not take second place to profit motives. Altering the human genome in a way that allows human-made genetic changes to be propagated throughout the population has a potential to alter the genetics of the human species as a whole.
Mary Faith
That raises the question of how long it will take for long-term effects to show. It’s one thing for an implanted egg not to survive. But how long will it take to know whether there are effects that aren’t obvious at birth?
Keith
We’re still collecting long-term outcome data for people born using different reproductive technologies. So far there have been no obviously horrible consequences. But some abnormalities could take decades to manifest, and there are many variables to contend with.
One can arguably say that there’s substantial good in helping couples have babies. There can be a benefit to their emotional well-being, and reproduction is a natural part of human health and biology. And a lot of really smart, dedicated people are putting a lot of energy into making sure that the risks are minimized. We can also look to some of the practices and approaches to oversight that have been used over the past several decades.
Mary Faith
And thinking about international guidelines, such as from the Council for International Medical Science and other groups, could provide guidance on protecting human research subjects.
Keith
You hate to advocate for a world where the automatic response to anything new is “no, don’t do that.” My response is, “Show me it’s safe before you do it.” I don’t think that’s unreasonable.
Some people have a view that scientists don’t think about the ethics of research and what’s right and wrong, advisable or inadvisable. But we do think about it. I co-direct a research training program that includes teaching scientists how to responsibly and ethically conduct research, including speakers who specifically address the ethics of reproductive technologies. It is valuable to have a dialogue between scientists and ethicists, because ethicists will often think about things from a different perspective.
As people go through their scientific careers and see new technologies unfold over time, these discussions can help them develop a deeper appreciation and understanding of the broader impact of their research. It becomes our job to make sure that each generation of scientists is motivated to think about these things.
Mary Faith
It’s also really important to include stakeholders – people who are nonscientists, people who experience barriers to reproduction and people who are opposed to the idea – so they have a voice at the table as well. That’s how you get good policies, right? You have everyone who should be at the table, at the table.![]()
Keith Latham, Professor of Animal Science, Adjunct Professor of Obstetrics, Gynecology and Reproductive Biology, Michigan State University and Mary Faith Marshall, Professor of Biomedical Ethics, University of Virginia
This article is republished from The Conversation under a Creative Commons license. Read the original article.